
BRITTLE DIABETES
Also known as labile diabetes, is a term used to describe a rare form of diabetes in which blood glucose levels are exceptionally difficult to control. Most often, it affects people with type 1 diabetes though it can very occasionally occur in those with a severe lack of insulin from other causes. The hallmark feature of brittle diabetes is the unpredictability and severity of blood sugar swings, with patients experiencing rapid transitions between extreme hyperglycemia (high blood sugar) and hypoglycemia (low blood sugar) often without a clear trigger.
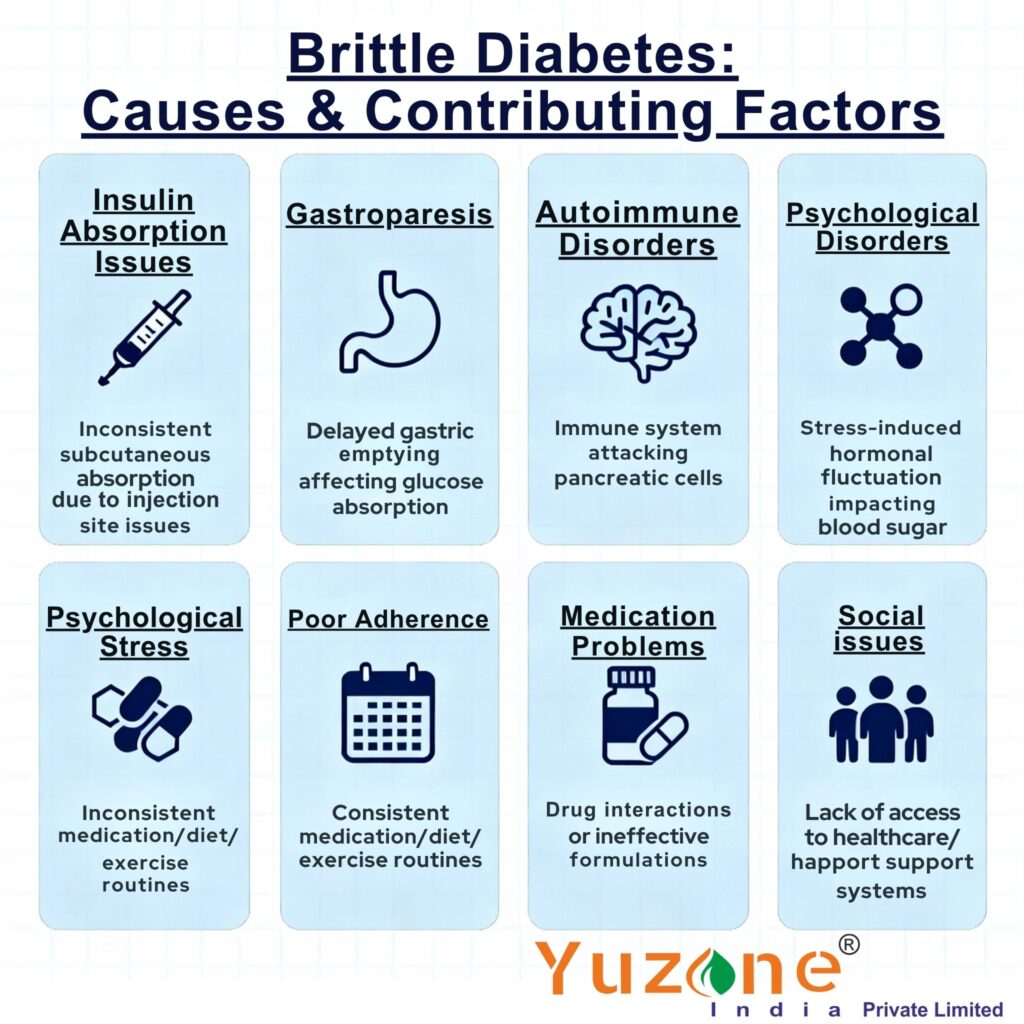
Several underlying factors can contribute to this instability. Physiological issues like insulin absorption problems, gastroparesis (delayed stomach emptying), celiac disease, hormonal imbalances, systemic infections, and certain autoimmune or endocrine disorders play a role. Psychological stress, psychiatric conditions such as depression and anxiety, as well as poor adherence to diabetes management plans significantly exacerbate blood sugar volatility. Additional contributors include memory loss, dementia, substance misuse, medication interactions, lipohypertrophy (fatty lumps from repeated insulin injections), and social issues like food or insulin insecurity.
People with brittle diabetes may present with highly elevated hemoglobin A1c values—indicating poor long-term glucose control—and are prone to emergency situations, including diabetic ketoacidosis (DKA) and hypoglycemic comas. Symptoms can manifest as confusion, sweating, heart palpitations, hunger, vision changes, impaired coordination, anxiety, and hypoglycemia unawareness, a dangerous condition where patients fail to recognize dangerously low blood sugar until it becomes severe. Research suggests that brittle diabetes is more common in females than males and especially in young adults, although it can affect people of any age and is less commonly seen after age 40.
Managing brittle diabetes is challenging and often requires an individualized multidisciplinary approach, including intensive glucose monitoring, psychological support, dietary modifications, and sometimes addressing underlying autoimmune or digestive disorders. Although technology such as insulin pumps and continuous glucose monitors can help, achieving stability remains difficult for those affected by this complex, multifactorial disease.



Comments are currently closed.